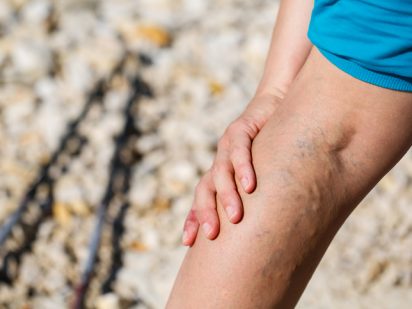
Healthy leg veins contain valves that open and close to assist the return of blood back to the heart. Varicose veins are veins that have become enlarged and twisted. According to the Society for Vascular Surgery, about 35 percent of the population in the United States can get varicose veins.
Venous reflux disease develops when the valves that keep blood flowing out of the legs and back to the heart become damaged or diseased. As a result, veins will not close properly, leading to symptoms of varicose veins, pain, swollen limbs, leg heaviness, and fatigue, skin changes, or ulcers.
They can be unsightly, but they can also be painful.
Varicose veins are genetic, said Jake Naidu, DO, an interventional radiologist with Trinity Health. Other factors include age, gender, pregnancy, obesity, and prolonged standing. For women, varicose veins can occur as early as their 20s, when a woman can be pregnant, Dr. Naidu added. “While they’re pregnant, the baby can put pressure on these veins.”
According to Mayo Clinic, visible signs of varicose veins include veins that are dark purple or blue in color, or veins that appear twisting and bulging, often like cords on the legs.
Additionally, painful signs and symptoms can occur, including:
- An achy or heavy feeling in the legs
- Burning, throbbing, muscle cramping, and swelling in the lower legs
- Worsened pain after sitting or standing for a long time
- Itching around one or more of the veins
- Bleeding from varicose veins
- A painful cord in the vein with red discoloration of the skin
- Color changes, hardening of the vein, inflammation of the skin, or skin ulcers near the ankle, which can signal a serious form of vascular disease that requires medical attention
Self-care, such as exercise, elevating the legs, or wearing compression stockings, can help ease the pain of varicose veins and may prevent them from getting worse. However, if you are concerned about how the veins look and feel, and the self-care measures haven’t worked, see your provider, Mayo Clinic suggested.
Taking care of varicose veins is important, as these veins “can worsen and cause significant morbidity and can lead to ulceration in advanced cases,” Dr. Naidu said. “If they’re left untreated, they can form ulcers that can’t heal.”
For years, vein stripping was the treatment for varicose veins, although it was rough on the patient. The procedure included an incision made in the groin and calf; a hook is threaded through the diseased vein to pull the vein out of the leg.
With the radiofrequency ablation (RFA) procedure, the likelihood of pain and bruising associated with vein stripping surgery becomes a thing of the past.
Before the RFA procedure is done, Dr. Naidu or a nurse practitioner will evaluate to see whether the patient is a candidate based on symptoms. If the individual is a candidate, an ultrasound will be done to show damaged veins.
Until there is documentation that confirms the veins are damaged, “we put the patient on a three-month regimen of conservative therapy,” Dr. Naidu said. After three months, if nothing has improved through conservative therapy, “we schedule the patient for the procedure.”
RFA is performed on an outpatient basis. For the procedure, an incision is made in the skin. Using ultrasound, Dr. Naidu positions a catheter into the diseased vein through the small incision. The tiny catheter powered by radiofrequency energy delivers heat to the vein wall. As the thermal energy is delivered, the vein wall shrinks, and the vein is sealed closed. Once the diseased vein is closed, blood will reroute itself to healthy veins.
Most patients report feeling little, if any, pain during the procedure. (A local or regional anesthetic is used to numb the treatment area.) Following the procedure, a simple bandage is placed over the insertion site, and an additional compression may be provided to aid healing. Your doctor may encourage you to refrain from extending standing and strenuous activities for a period of time. The average patient typically resumes normal activities within a few days.
Most patients report a noticeable improvement in their symptoms within one to two weeks following the procedure. Patients treated with RFA may resume normal activities more quickly than patients who undergo surgical vein stripping or endovenous ablation.
Trinity Health’s Interventional Radiology department includes Jake Naidu, DO; Heather Boyko, FNP-C; and Lynette Vondal, FNP-C.